What Is Major Depression Disorder
What Is Major Depressive Disorder (MDD)?
Understanding the Condition and the Hope for Healing
At Odinma Health, we believe healing goes beyond medication. We know that understanding what you’re going through is a powerful first step toward getting better. That’s why we’re taking a moment to talk about Major Depressive Disorder (MDD)—a condition that affects millions of people but is still often misunderstood.
What Exactly Is MDD?
Major Depressive Disorder, also called clinical depression, is more than just feeling down or having a rough day. It’s a medical condition that deeply affects how you think, feel, and function. It can interfere with daily activities, relationships, and your ability to experience joy or purpose.
People living with MDD often describe it as a heavy fog that just won’t lift—no matter how hard they try. And it’s not about being weak, lazy, or unmotivated. It’s a real condition that deserves real support.
Common Symptoms of MDD
MDD can look different for everyone, but some common symptoms include:
- Persistent sadness or low mood
- Loss of interest in things once enjoyed
- Fatigue or lack of energy
- Changes in appetite or weight
- Trouble sleeping or sleeping too much
- Difficulty concentrating
- Feelings of guilt or worthlessness
- Thoughts of death or suicide
For a diagnosis, these symptoms usually last at least two weeks and significantly impair daily life.
What Causes MDD?
There’s no single cause. MDD often develops from a combination of factors:
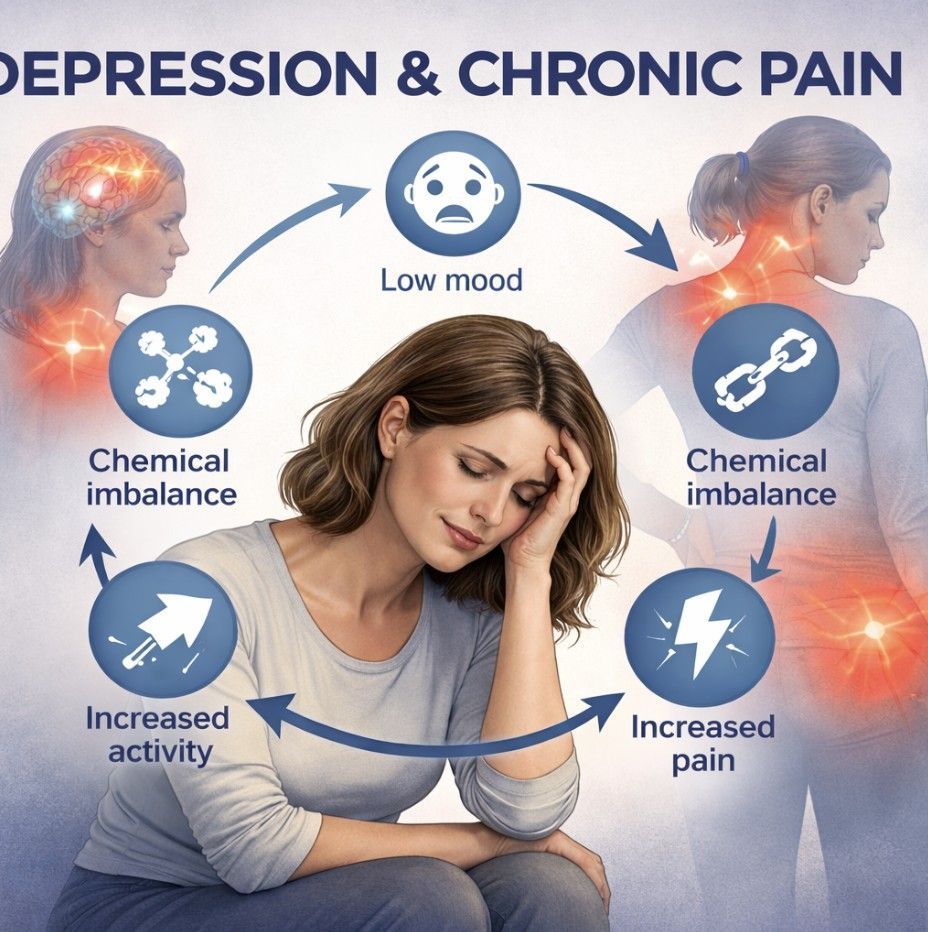
- Biological: Imbalances in brain chemicals or family history
- Psychological: Negative thinking patterns, trauma, or chronic stress
- Social: Isolation, life transitions, or lack of support
At Odinma Health, we look at the whole person, not just the symptoms. That means we consider your environment, your story, your stressors, and your strengths.
There Is Help—and There Is Hope
MDD is treatable. The most effective care plans are often holistic—combining medication (when appropriate), brief talk therapy, lifestyle changes, and coaching that helps you regain a sense of control over your life.
At Odinma Health, we walk with you through that journey. Our goal isn’t just to reduce symptoms—it’s to help you reclaim your joy, rebuild your routines, and reconnect with yourself. We also help you taper off medications when you’re ready and stable, because healing should feel like freedom, not dependence.
You’re Not Alone
If you or someone you care about is struggling with depression, know this: you don’t have to carry it alone. Seeking help is a courageous and empowering act. Whether you’re newly diagnosed or have been living with MDD for years, you deserve compassionate care tailored to your needs and goals.
Let’s work together to turn the page.
Ready to take the next step?
Book an appointment with Odinma Health today. Your healing matters—and we’re here to help you walk through it with clarity, care, and confidence.
Recent Posts